CHARCOT MARIE TOOTH
FOOT DEFORMITY
Over the past few years I have become more interested in the care of the charcot-marie-tooth foot since its such a difficult and many times debilitating condition. I’ve found that there is an unusual lack of foot surgeons experienced and comfortable treating this and getting functional results. I have been involved in CMT surgery for approximately 25 years and find it to be one of the most important surgical services our office provides. If you need help we would be honored to help you either by treating you ourselves or helping find a qualified doctor close to you.
WHAT IS CHARCOT MARIE TOOTH AND WHY DOES IT EFFECT THE LEGS?
CMT is a progressive neurological condition that essentially causes an imbalance between muscles in the legs. The first thing that happens to many people is a weakness that they notice when flexing the ankle upward. This can often be noticed most when walking up stairs or walking barefoot on level ground. When this weakness progresses, they can lose the ability to dorsiflex their foot altogether. This is called dropfoot ( or foot drop). This is very often the most common presentation. Also it’s not all of the leg muscles that get weak at the same time. CMT causes something called relative weakness . This means that the muscles on the outside of the leg weaken first, specifically the peroneus braves muscle in the leg . The other muscles may also develop weakness but not necessarily at the same time. After this occurs, weakness in certain muscles the foot can change shape.
Since it’s usually the peroneal muscles that weaken first the foot will begin to turn inward toward the other foot and then the arch of the foot will get higher. A high arch foot is called a cavus foot. At that point as the arch rises and muscle weakness continues the toes develop what we call a hammer digit or hammertoe. This is due to weakness in the very small muscles inside the foot called the intrinsic foot muscles.
Below is a classic picture of a charcot marie tooth foot. The muscles on the outside of the foot that pull the foot foot outward into whats called pronation- they weaken. The muscles on the inside of the foot that pull up the arch and turn the foot inward ( called supination) overpower the outside muscles ( peroneal muscles, there are two of them , the peroneus longus and peroneus brevis ) hence raising the arch. See the picture below.
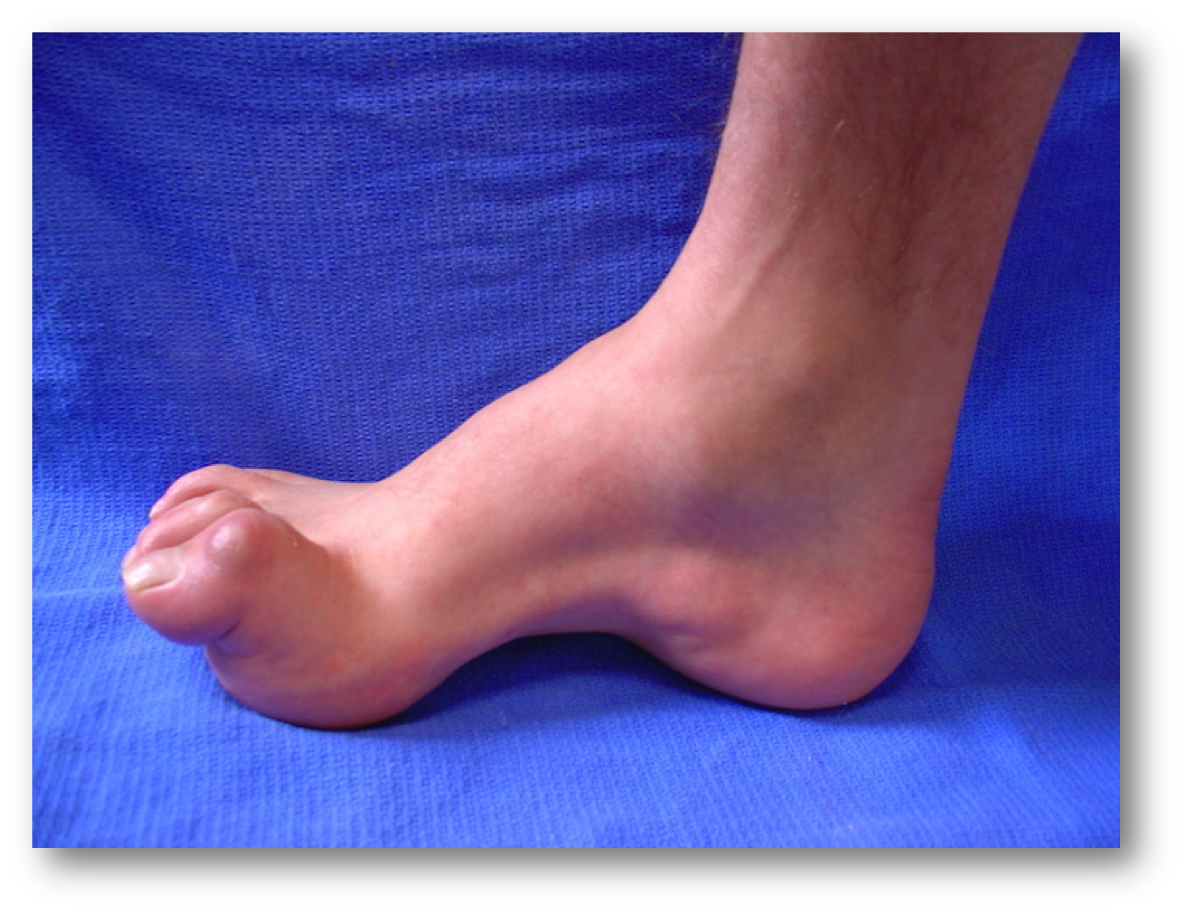
Now take a look at the image below, the heel is inverted or tilted inward ( the arrow points to the inside of the arch, we call that the medial side ). So as the arch increases in height the heel goes into an inverted position called a varus heel, this makes for an unstable foot during walking which makes the patient prone to ankle sprains. The higher the arch gets the more the heel inverts.

By understanding the above pictures and the reasons for those deformities to happen you will understand the surgical procedures we use to fix the foot.
To fix a CMT foot we need to address number of things:
the high arch - higher when the disease progresses
the inverted heel - goes with the high arch
dropfoot - weakness of the muscles that pull up the ankle
hammertoes of the lesser toes - weakness of intrinsic muscles
equinus - when 1-4 occur the achilles gets tight and prevents normal ankle motion
Hammertoe of the hallux ( big toe) its treated differently than the other toes ( Jones Teno-suspension)
A surgical plan is developed addressing each of those elements of the CMT foot. Of course every patient is different and a different combination of procedures may be necessary to create a functional foot.
THE SURGICAL PLAN FOR CHARCOT MARIE TOOTH FOOT:
In some cases patients come in with a severe high arch condition of the foot. In some instances we use an external fixator to stretch the foot back into a more correct position. And then we come back in for a second surgery to lock the new position in place with fusions of certain joints.
Sometimes people come with cavus high arch AND severe arthritis to the foot joints, in those cases we fuse the joints with a procedure called a triple arthrodesis. This limits the joint motion all together but puts the feet in a better position on the floor.
In the most optimal case we use something called an osteotomy. This is where we cut the bone to reposition and spare the joints.
HERE IS MORE IN DEPTH INFORMATION ABOUT HOW THE MUSCLES WEAKEN AND CAUSE A HIGH ARCHED CMT FOOT
WORK IN PROGRESS
To contact us for help please fill out the form below or call us.
OTHER CONDITIONS RELATED TO CHARCOT MARIE TOOTH FOOT
IF YOU HAVE QUESTIONS OR WOULD LIKE TO SEE US PLEASE CALL
212-372-0991 OR 239-465-0311
FREQUENTLY ASKED QUESTIONS ABOUT CHARCOT MARIE TOOTH FOOT CONDITION :
What is Charcot-Marie-Tooth (CMT) and how does it affect the feet?
Charcot-Marie-Tooth is a group of inherited disorders that cause progressive damage to the peripheral nerves, which are responsible for sending signals from the brain to the muscles and back. Because the longest nerves are often affected first, the feet and lower legs are typically the first areas to show symptoms like muscle weakness and atrophy. This nerve damage leads to a loss of muscle balance in the foot, which often results in the development of high arches, hammertoes, and an unstable gait. Over time, these structural changes can make walking difficult and increase the risk of frequent trips or falls.
Why do people with CMT often develop high arches (pes cavus)?
High arches, or pes cavus, occur in CMT because the disease causes an imbalance between the muscles that pull the foot in different directions. As certain intrinsic foot muscles weaken and atrophy, the stronger remaining muscles pull the foot into a high-arched position and cause the toes to curl into "hammertoes." This rigid, high-arched structure reduces the foot's ability to absorb shock and creates localized pressure points on the ball and heel of the foot. Without proper support or intervention, this deformity can lead to chronic pain, severe instability, and difficulty finding comfortable footwear.
What is "foot drop" and why is it common in CMT patients?
Foot drop is a condition where the muscles in the front of the leg become too weak to lift the front part of the foot while walking. In CMT, the peroneal nerve is often compromised, leading to weakness in the tibialis anterior muscle which normally performs this lifting motion. To compensate for the toes dragging on the ground, many patients develop a "steppage gait," where they lift their knees higher than normal to clear the floor. This lack of control over the foot significantly increases the risk of tripping, especially on uneven surfaces or thick carpeting.
When should I consider custom orthotics or AFO braces?
Custom orthotics or Ankle-Foot Orthoses (AFOs) should be considered as soon as you notice instability, frequent tripping, or persistent foot pain. Orthotics can help support a high arch and cushion pressure points, while AFOs are specifically designed to manage foot drop by holding the foot in a neutral position during the swing phase of walking. These devices not only improve safety by preventing falls but also reduce the energy required to walk, allowing for greater mobility and less fatigue. Consulting with a specialist early can help prevent the progression of deformities and keep you active for longer.
Is surgery necessary for CMT foot deformities?
Surgery is typically considered when conservative treatments like bracing, physical therapy, and orthotics are no longer sufficient to manage pain or maintain mobility. Common procedures include tendon transfers to rebalance muscle pull, osteotomies to realign bones, or joint fusions to stabilize a severely deformed foot. The goal of surgery is to create a "plantigrade" foot—one that is flat on the ground—to improve balance and make bracing more effective. Early surgical intervention is often recommended by specialists to prevent the deformity from becoming rigid and more difficult to correct later in life.
Why is daily foot inspection so important for CMT patients?
CMT often causes sensory loss or numbness in the feet, meaning you may not feel a blister, cut, or foreign object in your shoe. If left unnoticed, these minor injuries can quickly develop into deep ulcers or serious infections because the body's ability to heal may also be slightly compromised. By inspecting your feet daily with a mirror, you can catch redness or skin breakdown before it becomes a major medical issue. Consistent foot hygiene and professional nail care are also vital to prevent ingrown toenails and fungal infections that can lead to further complications.
Does CMT cause foot pain or burning and tingling sensations?
Yes, many people with CMT experience chronic foot pain due to structural deformities like high arches and hammertoes that create abnormal pressure points. The nerve damage itself can also cause neuropathic pain, described as burning, tingling, shooting, or electric-shock sensations in the feet and lower legs. Some patients experience cramping in the foot and calf muscles, especially after prolonged standing or walking. Pain management strategies include proper footwear, orthotics, physical therapy, and in some cases, medications specifically designed to treat nerve pain.
Why do I keep tripping or rolling my ankles with CMT?
Tripping occurs primarily due to foot drop, where weakened muscles can't lift the front of the foot high enough to clear the ground during walking. Ankle rolling and instability result from weakness in the peroneal muscles on the outside of the lower leg, which normally stabilize the ankle joint during weight-bearing. The combination of muscle weakness, high arches, and reduced proprioception (awareness of foot position) makes it very difficult to react quickly to uneven surfaces. AFO braces and high-top supportive footwear can dramatically reduce these incidents and improve confidence while walking.
Can CMT cause ankle instability and frequent sprains?
Absolutely—ankle instability is one of the most common and frustrating symptoms of CMT. Weakness in the peroneal and tibialis muscles reduces the ankle's ability to maintain proper alignment, especially during the push-off phase of walking or when navigating slopes and uneven terrain. Repeated ankle sprains can lead to chronic ligament laxity, making the joint even more unstable over time. Strengthening exercises, proprioceptive training, ankle braces, and in severe cases, surgical stabilization procedures can help restore function and prevent further injury.
Why is daily foot care important if I have numbness?
Reduced sensation means you may not feel a pebble in your shoe, a blister forming, or even a small cut that could become infected. In CMT, minor injuries can quickly escalate into serious problems like deep ulcers, cellulitis, or bone infections because the warning signal of pain is absent. Daily inspection with a mirror allows you to catch redness, swelling, skin breakdown, or foreign objects before they cause significant damage. Keeping feet clean, moisturized, and protected with proper footwear is essential to preventing complications that could lead to hospitalization or even amputation in extreme cases.
What foot problems should I watch for (calluses, ulcers, nail issues)?
Common problems include thick calluses on pressure points (ball of foot, heel, or toe tips) that can break down into painful ulcers if not managed. Ingrown toenails are frequent due to toe deformities and improper trimming, and fungal infections thrive in the warm, moist environment between curled toes. Swelling (edema) in the feet and ankles can indicate circulatory issues or overuse, while any open sores, drainage, or foul odor signals a potential infection requiring immediate medical attention. Regular visits to a podiatrist familiar with CMT can help identify and treat these issues before they become serious.
What are the best shoes for CMT and cavus foot?
The ideal shoe should have a wide, deep toe box to accommodate hammertoes without causing friction or pressure sores. Excellent cushioning and arch support are critical to redistribute pressure away from the ball and heel, where high arches concentrate weight. A firm heel counter and high-top design provide lateral ankle stability to prevent rolling, while rocker-bottom soles facilitate a smoother gait when ankle motion is limited. Avoid shoes that are too tight, too loose, or have thin soles, and always break in new footwear gradually to prevent blisters.
Do I need custom orthotics for CMT?
Custom orthotics are highly recommended for most CMT patients because over-the-counter inserts rarely provide adequate support for the unique combination of high arches, pressure points, and instability. A custom orthotic is molded specifically to your foot shape and can include features like deep heel cups, metatarsal pads, and arch fills that redistribute pressure and improve alignment. They work best when paired with supportive footwear and should be re-evaluated periodically as your foot structure changes. Many patients report significant reductions in pain and fatigue after being fitted with properly designed custom orthotics.
When should someone with CMT consider custom shoes?
Custom shoes become necessary when foot deformities are so severe that even extra-depth or wide shoes cannot accommodate the shape without causing pain or skin breakdown. Patients with extreme high arches, rigid hammertoes, or significant leg-length discrepancies often benefit from fully custom-molded footwear. Custom shoes can be designed to work seamlessly with AFO braces and orthotics, providing a complete support system. While they can be expensive, many insurance plans cover custom therapeutic footwear for patients with documented neurological conditions like CMT, especially if there is a history of ulceration or infection.
What exercises or physical therapy help CMT foot and ankle problems?
Physical therapy for CMT typically focuses on stretching tight structures (like the Achilles tendon and toe flexors), strengthening remaining functional muscles, and improving balance and proprioception. Exercises may include calf stretches, toe spreads, ankle alphabet exercises, and resistance band work for the peroneal and tibialis muscles. Balance training on wobble boards or foam pads can help reduce fall risk. A physical therapist familiar with CMT can design a program that maintains flexibility and strength without overworking muscles, which can sometimes accelerate weakness in neuromuscular conditions.
Can stretching (like Achilles stretching) help cavus or tightness?
Yes, regular Achilles tendon stretching is one of the most important self-care activities for CMT patients with high arches. A tight Achilles tendon pulls the heel upward and exacerbates the cavus deformity, increasing pressure on the ball of the foot and making walking more difficult. Gentle, sustained stretches performed multiple times daily can help maintain ankle flexibility and reduce the progression of contractures. Stretching the plantar fascia and toe flexors is also beneficial for preventing hammertoes from becoming rigid. However, stretching should be done carefully and never to the point of pain, as overstretching can cause injury.
When is surgery recommended for CMT cavus foot?
Surgery is typically recommended when conservative treatments like orthotics, bracing, and physical therapy no longer adequately control pain or maintain functional mobility. It's often considered when the foot deformity becomes rigid and fixed, making it difficult to fit into braces or shoes, or when severe instability leads to frequent falls and injuries. Many specialists advocate for earlier surgical intervention—ideally while the deformity is still flexible—because outcomes are generally better and recovery is faster. The decision to pursue surgery should be made collaboratively with an orthopedic surgeon experienced in CMT foot reconstruction.
Is it better to treat CMT cavus foot earlier rather than later?
Yes, early intervention is strongly recommended by most CMT specialists because flexible deformities are much easier to correct and have better long-term outcomes than rigid, fixed deformities. When treated early with orthotics, bracing, and sometimes minimally invasive procedures, progression can often be slowed or halted. Once the bones, joints, and soft tissues become rigidly deformed, more extensive surgery is required, recovery is longer, and the risk of complications increases. Regular monitoring by a foot and ankle specialist allows for timely intervention before deformities become severe and disabling.
Does CMT get worse over time, and will my foot deformity progress?
CMT is a progressive condition, meaning symptoms typically worsen gradually over many years or decades. The rate of progression varies widely between individuals and even between different types of CMT. Foot deformities like high arches and hammertoes tend to become more pronounced over time as muscle imbalance continues, and what starts as a flexible deformity often becomes rigid without intervention. However, with proactive management including appropriate bracing, orthotics, physical therapy, and timely surgical correction, many patients maintain good mobility and quality of life throughout their lives.
When do CMT symptoms usually start (and why do feet show it first)?
CMT symptoms most commonly begin in childhood or adolescence, though some types don't manifest until adulthood. The feet and lower legs show symptoms first because they contain the longest nerves in the body, and longer nerves are more vulnerable to the effects of CMT. Early signs often include “clumsiness”, frequent tripping, difficulty with sports or running, and the gradual development of high arches. Some children are diagnosed after parents notice unusual shoe wear patterns or an awkward gait, while others aren't diagnosed until symptoms become more pronounced in the teenage years or early twenties.
What should I do if I notice a sore, infection, or wound on my foot?
Any open wound, sore, or sign of infection (redness, warmth, swelling, drainage, foul odor) should be evaluated by a healthcare provider immediately—do not wait to see if it heals on its own. Clean the area gently with mild soap and water, apply a sterile dressing, and keep weight off the affected foot as much as possible until you can be seen. Because CMT patients often have reduced sensation and may have compromised healing, even small wounds can quickly become serious infections that spread to deeper tissues or bone. Early intervention with proper wound care, antibiotics if needed, and offloading pressure can prevent complications that might otherwise require hospitalization or surgery.
LOOKING FOR A SPECIALIST IN FLORIDA ?
VISIT OUR FLORIDA CMT OFFICE
LOOKING FOR A SPECIALIST IN NEW YORK?
VISIT OUR NYC CMT OFFICE
Our Florida and New York Office Locations
NAPLES OFFICE (Gulf Coast)
Serving Southwest Florida, including Fort Myers, Cape Coral, Bonita Springs, and Sarasota.
Address: 3940 Radio Road, Unit 104, Naples, FL 34104
Phone: 239-465-0311
WESTON OFFICE (Atlantic)
Serving the Tri-County area, including Miami, Boca Raton, West Palm Beach, and Hollywood.
Address: Weston near Cleveland Clinic coming soon
Phone: 239-465-0311
NEW YORK CITY OFFICE
Serving New York City and the boroughs as well as the entire Tri-state area
Address: 330 W. 58 street, Unit 610, NYC, NY 10019
Phone: 212-372-0991